The Plague of Pain

It’s an epidemic. As chronic pain sufferers search for relief, 2015 alone saw more than 20,000 opiate overdose deaths, almost double the number of heroin overdoses. But even as opioid abuse numbers skyrocket, many feel like they’re out of options. We spoke to local experts to explore pain management alternatives to pills and surgery.
The statistics on pain and pain remedies in America are enough to make anyone wince.
In 2011, the Institute of Medicine estimated 100 million U.S. adults suffered from chronic pain, the kind that springs from injury, disease or a short-circuiting of the nervous system. Chronic pain can last days, weeks, even indefinitely, bringing on depression and in extreme cases, shortening lives.
Dr. Carlos Roman, CEO of Southern Regional Anesthesia Consultants in Little Rock, focuses his medical expertise and professional will on the subject of pain management, helping patients better understand pain’s physiological and psychological components and ramifications.
“There is a realization that as we get older, we get physically limited. Sometimes we have a hard time coming to grips with that,” he says. “There’s a sense of people wanting to continue doing what they’ve done and they have to realize that medicine and pain medications have a limit on what they can and can’t do.”
Despite this, drug prescriptions have skyrocketed during Roman’s 20 years in this field. Physicians who maintained strict rules about prescribing pain medication were until very recently the exception, rowing upstream against billions in drug company marketing, unscrupulous pain clinics and doctors who were acting in good faith but on bad information. Even now, pain management decisions are fraught with ethical dilemma.
“[Patients] come in and say something’s hurting, you don’t just say ‘Oh, you’re a drug seeker, you’re full of it,’” Roman says. “You can’t do that. You have to realize there are things that end up being subjective like when the patient tells you this hurts.
“But then you get the guy who’s got the broken leg that’s healed, he’s supposed to be doing fine, why is he still having pain? That becomes a very complicated issue. I have to remind the patient it’s a pain management clinic, and the key word is ‘management.’ It’s not always a pain cure clinic.”
Roman also sits on the state’s Medical Marijuana Commission, and despite holding a healthy marijuana skepticism, he’s keeping an open mind learning about other states where pot is legal and opiate use has correspondingly declined.
“That’s going to be an interesting trend, hopefully involving good, adult discussion without too much fear-mongering on either side,” he says.
As millions of Baby Boomers move into their golden years and younger generations look for ways to get relief without meds, the field of pain management in all of its forms continues to grow. Management options in Arkansas range from very familiar to fringe and everything in between in the quest to be pain-free.
PHYSICAL THERAPY
No region of the body is more maligned by chronic pain than the lower back. According to the Low Back Pain Program, 95 percent of the general population experiences a severe episode of low back pain once in their lifetime, 85 percent will have recurring episodes and of this latter group, one-third to one-half will experience no resolution to their issue.
Bo Renshaw of Harris & Renshaw Physical Therapy in Little Rock said his clientele mirrors these statistics.
“If you include neck along with back, it’s easily 35 to 40 percent of our practice,” he says. “It’s by far the number one diagnosis group that we see.”
Physical therapy seeks to correct imbalances in the supporting structures of the body using various techniques and physical movements to strengthen a specific muscle group, thereby restoring the patient’s musculoskeletal integrity.
“A lot of physicians will recommend exercise, yoga and other things like that, and those are good,” Renshaw says. “But a physical therapist is going to be able to isolate a movement-impairment syndrome with something that’s specific to a particular muscle that has a deficit and needs to be corrected.”
Physical therapy is commonly prescribed for patients recovering from surgery, injury or accidents as part of pain management and increasingly applied in the creation of wellness programs.
“There’s a lot of research that shows early intervention with physical therapy has a higher outcome on resolution of low back pain and return to work,” he says. “We educate primary care physicians, orthopedic and neurosurgeons and the public to let people know that. We also go out on a regular basis to different industries to evaluate their ergonomic positioning and how they can not only protect their back, but protect all of their joints in the workplace.”
ACUPUNCTURE
Discussing the primary concerns people have of acupuncture, Martin Eisele of Little Rock’s Evergreen Acupuncture gets right to the point.
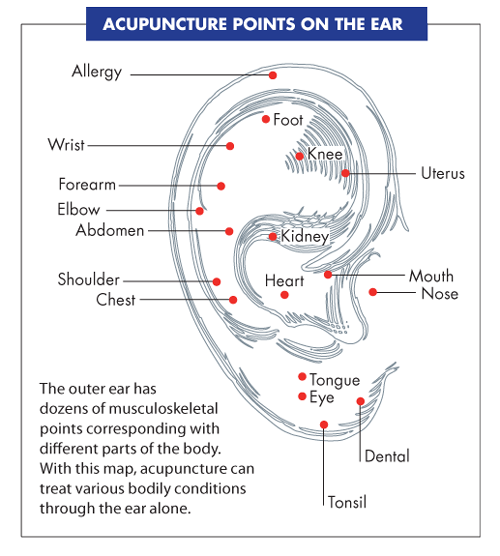
“One of the biggest drawbacks to getting people into my clinic is the idea of needles,” he says. “Even people with tattoos or piercings have this misconception about being jammed with needles. But the needles are real tiny, you can barely feel them and once they’re in, you don’t feel them at all.”
Acupuncture manipulates the flow of energy within the body through the insertion of needles at specific points. After being treated himself for low back pain, Eisele got so interested in the ancient medicinal practice he completed 4,000 hours of training to become licensed and has been in practice for 14 years.
“I’ve treated a kid that was three months old; I’ve treated somebody that’s 100 years old,” he says. “Treated a 12-year-old kid today and a 93-year-old woman last week. It goes back and forth.”
Eisele finds greater acceptance today by so-called “established” medicine as evidenced by the number and variety of referrals he gets treating not only pain, but fertility, digestive issues and more.
“It’s getting to be more and more popular,” he says. “I have a number of physicians that send me patients, a number of OB/GYN’s that send me patients. I had somebody come from their neurologist after the neurologist suggested acupuncture.”
Another key demographic is athletes either looking to recover from injury or to simply stay in peak form.
“I treat runners, yoga people, weekend warriors, high-endurance athletes,” he says. “A lot of people don’t really know that it can help with athletic performance. But if you reduce the stress, you can increase the endurance. And in cases of injury, you can increase recovery and healing.”
PAIN CLINIC
For all the positives Dr. Amir Quereshi has seen in the field of pain management over the past 12 years, there have also been spates of negative publicity stemming from a few high-profile bad actors.
“When we opened the doors, there were not as many restrictions or regulations or being under scrutiny by the feds on pain management,” he says. “Then there was a whole scam of pain clinics in Florida, and that’s where it all started. People just kept opening these pill mills and it got noticed that this is something bad going on.”
Even though Quereshi, like all reputable pain management clinics, has to live with regulatory and insurance fallout from these cases, his practice is a far cry from the scam artists who saw patients just long enough to write them a prescription.
“I have to explain [to patients] look, this doesn’t mean that you’re coming here for just narcotics business or medication business,” he says. “If you come to me with back pain, I will of course figure out where this pain is coming from. I would need some X-rays, I would look into the history of why this happened, just like any other doctor. And then from there we make a treatment plan.”
That plan may include various physical therapies, bracing, electrical stimulation or surgical procedures, many of which are far less invasive than previous versions. And while medications are prescribed under the appropriate circumstances, Quereshi said it’s by no means a given that drugs will be part of the treatment.
“There are a lot of patients, good patients, they don’t want [drugs] so they’re even scared to walk into a pain clinic,” he says. “We just calm them down and tell them ‘Look, different options are available.’”
THERAPEUTIC MASSAGE
Arkansas Healing Arts Massage and Wellness may look like any other massage business in Little Rock, but don’t let appearances fool you. When it comes to therapeutic massage, Kate (Li-Chu) Nicoletti and the rest of the therapists aren’t all scented oils and soft music.
Nicoletti’s 90-minute sessions are intense and effective, particularly when taken regularly. Her established clientele trends older, but she’s also been sought out by college athletes during her 12-year career. A figure skating client even took Nicoletti on the road with her to major competitions.
The hours of classroom work required to earn and maintain credentials continually challenges her to hone her skills, but it’s the hours in the treatment room that taught her to read her clients from the first touch.
“People often come to me not necessarily for pain, but because they feel tight,” she says. “Well, they think it’s because they’re aging, they’re supposed to be that way. No, actually you always can change and feel better.”
It’s important to have the correct expectation for therapeutic massage, which is about repair and healing, not mere relaxation. Each treatment is exactly that — treatment — and communication is paramount. Don’t judge the therapist by their appearance; when they say “firm pressure,” they’re not kidding. But an experienced massage therapist such as Nicoletti will constantly ask for feedback as the session goes along, and the more information you give, the better the end result.
“Unless you are in the medical field and are a person who knows the body a little bit more, like a personal trainer, you have no idea how the body works. All you know is just where’s the pain,” Nicoletti says. “A lot of things I can just tell by working the muscle, but I also have my clients tell me things so I can find the problem.”
CHIROPRACTIC MEDICINE
Among the more familiar pain management treatments is chiropractic medicine, which focuses on keeping the body in alignment so muscles, ligaments and other structures can function as intended.
Chiropractic medicine was once almost taboo, but now far more unease surrounds prescription drugs. (Photo: Little Rock Athletic Club)
“Musculoskeletal pain is often due to mechanical causes,” says Dr. Bev Foster of Chiropractic Health and Rehabilitation. “Mechanical causes mean the pain is not caused from an infection, some kind of cancer or disease process in the skeletal system. Rather, it’s some kind of derangement, some kind of imbalance, whether it’s muscle strain or ligament sprain or a loss of joint motion in play.
“There really aren’t any drugs that treat the mechanics. Chiropractic manipulation is the core therapy that most chiropractic physicians and osteopathic physicians practice. Manipulation is mechanical treatment for mechanical problems.”
Chiropractic medicine hasn’t always been in favor with the medical establishment, but times have definitely changed, particularly as the pain management field has grown and with the overall skittishness many patients now have toward medication.
“Most people are fairly reluctant to take an opiate, and many people are starting to experience the long-term effects of NSAIDs where they’ve been taking ibuprofen or Aleve every day, too,” Foster says.
Still, she noted that doesn’t mean every patient she sees is 100 percent pain pill-free. In fact, some have been referred to her practice as part of being weaned off of opiates.
“Conventional medicine is just getting on the bandwagon as a result of what’s being called the opiate epidemic,” she says. “From my perspective, [pain treatment] is upside down.They should have been treated conservatively first and they weren’t and they became addicted.”
“But now, not only do I think it’s upside down, the American College of Physicians thinks it’s upside down, and they are coming out very strongly with recommendations for not jumping on these drugs until it’s a last resort.”
YOGA
David Shropshire’s motivation for getting into yoga started with a desire to help people, specifically an aunt with dementia. Today, he combines the benefits of yoga, natural movement and personal training at Clubhaus Fitness in Little Rock.

“[Yoga’s] all about activation.” - David Shropshire (Photo: Miranda Yelvington)
Shropshire said combining yoga with these other disciplines provides complementary pain management benefits over performing one activity exclusively, leading to the myriad variations of yoga sessions he leads.
“When you go into yoga, your intention for the practice can dictate where your practice goes,” he says. “I teach some hot yoga classes that are more athletic-based and more focused on strength, stability, core work, all that kind of stuff.
“If you go into the class and your intention is just to be able to move better, that changes the mindset of what we’re going to do.”
Shropshire says yoga isn’t the fringe activity it used to be, but many misconceptions still exist.
“One of the things I generally tell people is yoga is not stretching,” he says. “When people start thinking stretch they think inactivity. Unfortunately, a lot of us tend to not really be aware of what we’re doing and rest on connective tissue — sinking into the back, legs locked out — on a pretty regular basis. If you have somebody in a class thinking they’re there to stretch, the same thing happens, just in a more peaceful setting.
“The way that I teach, it’s all about activation. What’s happening is you’re using the muscles to help move you deeper into that alignment, deeper into the posture. If I’m really working on my alignment and I’m active, that’s going to allow me to move into the posture more effectively, which is going to dictate how efficient my movements are.”
MEDICATION NATIONIn years gone by, drug addicts were largely identified in the public consciousness as people taking something illicit. But the nation’s current struggle with opiates is perhaps most insidious for the fact it stems from something legal, created to bring relief and still commonly prescribed by doctors. “I never bought into the mantra of giving patients lots of opiates for chronic, non-cancer pain. It just flew in the face of basic physiology and pharmacology you study in medical school,” said Dr. Carlos Roman of Little Rock, a leading pain expert.  “I tell patients all the time, I’m a horrible salesperson but I try to be a good doctor. I wish I could tell you if I give you more morphine you’re going to feel better, but you’re just going to get more physically dependent, you’re going to get more tolerant, and it’s going to work less and less.” Over the past few years the U.S. Centers for Disease Control issued prescribing guidelines preaching restraint on opiates, but there’s ample evidence that such measures are chasing a runaway train. The U.S. is estimated to consume a staggering 80 percent of the world’s opiates supply, despite having just five percent of the world’s population. Drawn from the same pharmaceutical category as heroin, opiates include the highly addictive drugs oxycodone, hydrocodone and morphine. In one recent study 80 percent of heroin users said opiates were their gateway drug. Another report revealed six percent of patients with a one-day supply of opioids were still taking the drug a year later. Twelve percent of patients prescribed a six-day supply and 24 percent of those given an initial 12-day supply were still taking the meds a year later. As if that weren’t shocking enough, the American Society of Addiction Medicine reported more than 20,000 opiate overdose deaths in 2015, almost double that of those dying from heroin overdose. Roman says the lucrative nature of the pain pill business, deeply ingrained medical beliefs and residue of the prescribe-first, worry-later attitudes in some corners of the pain management community have made change slow in coming. “Unfortunately, when economics get with medicine you see problems like these come up, and this is a multi-billion dollar industry,” he said. “It’s also kind of a hard pill to swallow when the CDC comes out and says, ‘Hey, you guys got this wrong,’ so there’s still doctors out there prescribing significant amounts of narcotics even though the true science is not behind it. “The money involved and changing economic model to get into what I call a proper practice of pain management is an ongoing fight.” |







